
Cervical Screening &
Human Papillomavirus (HPV)
Below you’ll find information about HPV, cervical screening and how self‑collect testing works at Clinical Labs.
-
Self-Collect HPV Testing
What is self-collect HPV testing?
Self‑collect HPV testing allows patients to collect their own sample for cervical screening. It offers a comfortable and private option suitable for many people. Benefits include:
- Comfortable and private
- Quick and convenient
- Safe during pregnancy
- As accurate as clinician-collected samples
Who is eligible for self-collect HPV testing?
Self‑collect HPV testing can be offered every 5 years to:
- Women or people with a cervix aged 25 and 74 who are due or overdue for cervical screening, including during pregnancy
- Patients who are not symptomatic for cervical cancer (see symptoms below)
- Patients at other points in the cervical screening pathway when only an HPV test is required, including test of cure after treatment for high-grade squamous intraepithelial lesion (HSIL)
- Patients who have had a total hysterectomy with history of HSIL
Patient groups not eligible for self-collect HPV:
- Patients who have signs and symptoms suggestive of cervical cancer (see below)
- Patients undergoing surveillance after a completely excised adenocarcinoma in situ (AIS)
- Patients with in-utero exposure to Diethylstilbestrol (DES)
If you are due or overdue for your 5-yearly cervical screening test, speak to your doctor about whether self-collect HPV testing is right for you.
-
Self-Collect HPV Testing Instructions
Self-Collect Patient InstructionsItems required for self-collect:
- Clinical Labs request form signed by your doctor (ensure self-collect HPV test is noted).
- Copan FLOQSwab® for vaginal self-collection (552C) (red-top dry swab) – available from
Clinical Labs.
Only Copan FLOQSwab 552C is validated for use.

Steps for self-collection:
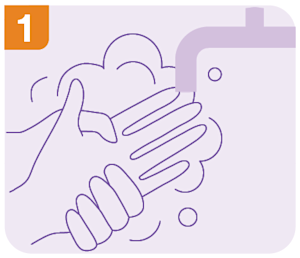
Before you collect your sample, ensure you have clean hands. To avoid contamination, do not remove the swab from the container until you are ready to collect your sample and do not use any lubricant.
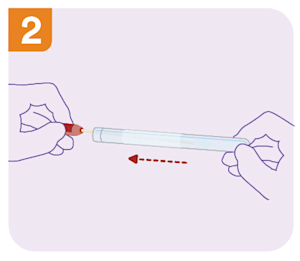
Once you are comfortable, remove the red cap and pull the swab out of the container.
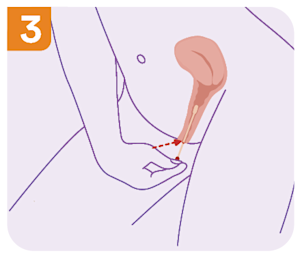
There is a red line halfway along the swab. Insert the front part of the swab inside your vagina, aiming for this red line.
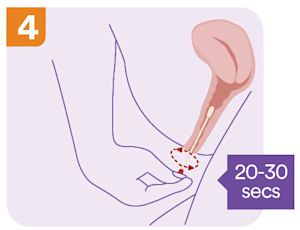
Once the swab is correctly inside your vagina, rotate it gently in a circular motion for 20-30 seconds.
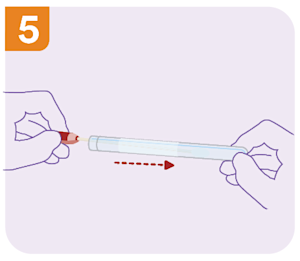
Remove the swab, place it back in the container and gently secure the cap.
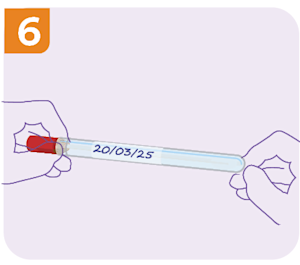
Return the self-collect swab and signed request form to your medical practice or Clinical Labs collection centre with priority. Please ensure the Collection Date is labelled on the container.
-
Cervical Screening and HPV
What is HPV?
Human Papillomavirus (HPV) is a common, often sexually transmitted viral infection that can cause genital warts and several types of cancer, including cancers of the cervix, vulva, vagina, penis, anus and some head and neck cancers. However, not all HPV infections lead to cancer. Most people with HPV do not have symptoms, and the virus often clears on its own.
There are many different types of HPV. Low-risk types may cause genital warts and minor changes in the cervix. High-risk types can sometimes cause precancerous changes and cervical cancer.
Women and people with a cervix aged 25 to 74 are encouraged to have a Cervical Screening Test (CST) every five years to check for HPV. Even if you are HPV vaccinated, it is still recommended to have a routine CST because the vaccine does not protect against all HPV types.
What are the symptoms of HPV?
Most patients with HPV do not have any symptoms. They usually do not develop warts and are often unaware they have the infection. Those that do develop warts on their body or genital area and may notice symptoms such as itching, discomfort, or flat, raised, single or clustered lesions.
HPV may be present in the body for several years before it causes changes in the cervical cells that are detected through pathology testing.
A Cervical Screening Test is the only way to determine if HPV is present.
How is HPV diagnosed?
HPV is diagnosed through a Cervical Screening Test (CST). Your HPV result helps your doctor determine whether you need further investigation or routine ongoing screening.
There are three risk categories:
- Low risk – routine re-screening in five years.
- Intermediate risk – repeat HPV test in 12 months to check whether the infection has cleared.
- Higher risk – referral to colposcopy for further investigation.
What are the HPV testing options?
Patients have two options for HPV testing:
- Clinician-collected samples (including for Liquid Based Cytology/LBC or ThinPrep®)
- Self-collected samples (dry swabs)
Note: If HPV is detected on the self-collect dry swab, the patient will need a clinician-collect sample so that LBC can be performed.
-
Cervical Cancer Information
What is cervical cancer?
Cervical cancer develops in the cells of the cervix. It is most commonly caused by a long‑term infection with certain types of HPV.
How common is cervical cancer?
The estimated rate of cervical cancer in Australia in 2025 was 6.7 cases per 100,000 women, which is among the lowest in the world.1
Staying up to date with your cervical screening tests is one of the most effective ways to help prevent cervical cancer.
Australia maintains low rates due to:
- HPV vaccination since 2007
- HPV-based cervical screening every 5 years
- Introduction of HPV self‑collection since 2022
Australia is recognised as being on track to become the first country to eliminate cervical cancer as a public health issue. Elimination is defined as fewer than 4 cases per 100,000 women each year.2
What are possible signs and symptoms of cervical cancer?
Speak to your doctor if you experience any of the following:
- Post-menopausal bleeding
- Unexplained bleeding between periods
- Persistent bleeding after sexual intercourse
- Unexplained abnormal vaginal discharge
If you have any of these symptoms, book an appointment with your doctor for assessment and to rule out cervical disease.
Related Pages
Sexual Health Testing
Learn about symptoms, testing, and treatment for syphilis, chlamydia, gonorrhoea and other STIs.

Preparing For Your Test
Prepare for your pathology test with essential information on fasting requirements, patient support and specific test instructions.

FAQ
Find answers to common pathology test questions, including preparation, fasting guidelines, collection centre locations, opening hours and aftercare tips at Clinical Labs.
